Augmented reality and medicine, is the Middle East ready?
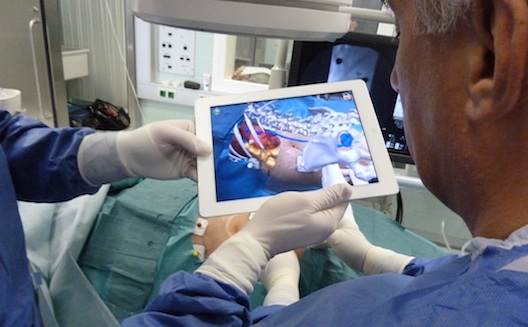
After-surgery care in developing countries or remote locations can often be an unknown quantity, but the use of augmented reality during operations could change this.
In April, medical journal The Lancet released a report that said up to two thirds of the world’s population has no access to safe and affordable surgery, and procedures such as removing an appendix or labor were the leading causes of death globally.
Increasingly, there are options - the most exciting of which is the use of augmented reality (AR) in the operating theater - that are making statistics such as those from The Lancet, a thing of the past.

Move over to the Middle East and several countries within this region are engulfed in conflict. Syria alone is reported to have lost over 460 medical professionals since 2011, according to Physicians for Human Rights.
Even if a victim is transported to a hospital and receives surgery, post-operation follow-ups with the patient dwindle once they are discharged. So, how can the situation be improved?
Augmented reality
AR is not an exclusive format for video gamers nor the sole marketing tool of furniture stores, and it could totally transform the world of medicine in both training and practical aspects.
For those unsure how AR works, the basic idea is that graphics, along with audio and other sensory enhancements, are superimposed onto a real-world environment in real time.
An elaborate explanation of how AR works. (Video via Ted Talks)
For example, if you wanted to know what a sofa might look like in your lounge you could use a phone or tablet to ‘create’ a fictional one in your line of vision, giving the illusion of it really being there.

Shortages and teaching - a solution
According to The Lancet study, there are 143 million simple operations that need to be performed annually, requiring 2.2 million staff. An application like AR telehealth startup VITAAX is one way in which these issues can be addressed.
Talal Ali Ahmad, the founder of VITAAX, started using AR when he began working with the international charity Global Smile Foundation three years ago. Seeing the work of surgeons fixing the cleft palates and lips of ‘underserved’ children, Ali Ahmad saw a major problem: the doctors would do their operations and move on, leaving behind sick children who still needed - but didn’t receive - continuing post-op care.
Talking to Wamda from his base in Boston, the electrical engineer said doctors or medical staff in the field were often resorting to talking to surgeons elsewhere by phone or over Skype, when it came to following up with patients.
As a result Ali Ahmad came up with a solution that could be used for both post-op care and actual operations.
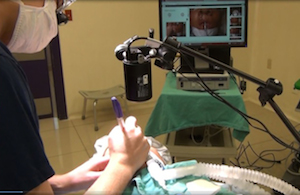
(Image via VITAAX)
“I built a software prototype and worked with surgeons to define the features they needed,” says Ali Ahmad. During initial field testing the operating surgeons would wear a Google Glass, which would overlay an AR image over the area being operated on.
The remote surgeon in New York city, with a laptop, would guide the local surgeon using direct drawing on his/her laptop which would then be transmitted to the operating surgeon’s computer or TV.
The second option, currently under development is the remote surgeon using a hi-def camera pointed at their hand. This way the software will merge the remote surgeon’s hand and the video of the patient. This image would then be projected onto the operating surgeon’s computer or TV.
At the same time medical wearable devices are attached to the patient in order to capture vital signs, or medical information, needed during the operation.
Initial field testing was done in Ecuador and El Salvador and in 2014 the Global Smile Foundation and Ali Ahmad began talking to Ghassan Abu Sitta, a surgeon at Lebanon’s American University of Beirut Medical Center (AUB MC).
The very modern teaching aid
AR is already being used in other countries as a cost effective teaching tool for surgical students.

An example is the application Touch Surgery, which awards scores for accuracy and knowledge, allowing surgeons to practice procedures that range from heart surgery to carpal tunnel operations.
It was created by another Lebanese expat, UK-based plastic surgeon Jean Nehme. He told Wamda they recently translated the app into Spanish and Chinese, adding that most medical students and staff in the Middle East were operating in English.
In the US, applications such as SimX apply AR as a teaching tool for surgery.
While there are no real stats available on how much the use of medical AR is worth, or could be worth, San Francisco-based consultancy Digi-Capital estimates that the fields of AR and VR (virtual reality) will hit “$150 billion by 2020, with AR taking the lion’s share [of the revenue] around $120 billion”.
Earlier this year Facebook Inc bought Oculus, the California-based company that created virtual reality headset Rift. Apparently looking 5 to 10 years into the future for the device’s use, Mark Zuckerberg said: “We’re going to make Oculus a platform for many other experiences…”, one of those being talking face-to-face with your doctor.
As a plastic surgeon, Abu Sitta sees the use of AR as ideal for his field. They are now planning on using the application in two other regional hospitals, one of those being Al-Shifa Hospital in Gaza.
In the aftermath of the 2008/9 Gaza war, Abu Sitta saw the value of online/remote practices when it came to medicine. “We tried to set up training programs for doctors there,” he told Wamda. “Because of the siege the only ones that really worked were the internet-based ones.”
As for cost, Ali Ahmad estimates the price of the VITAAX application will be about $1,500 to $2,500 a month, after an initial $2,500 setup fee.
A very new concept
While the use of AR in the medical sector might still be a new idea, it is being swiftly adopted in the region for its other uses.
“We’ve been very active,” says Dubai-based Pixelbug founder and CEO Dany El Eid. Having recently brought out their children’s AR edutainment application Colorbug, he tells Wamda that the activity in the space has been been picking up but that it’s still a nascent field, believing 2016 to be the year it really grows.

“It’s not a technology that is widely available, it’s highly specialized and prices will vary depending on the complexity of the app,” says El Eid. While not working specifically for medical clientele, Pixelbug were commissioned to create a fully customized AR for global pharmaceutical company Boehringer Ingelheim.
In Dubai the accelerator Turn8 is currently working with a Georgian startup called InGlove: it’s an interactive glove that allows the user to move their hands around and feel the shape of objects that appear in a computer simulation.
InGlove’s Dimitri Tskhovrebadze told Wamda that from his experience in the region the UAE in particular “is extremely interested in AR/VR [virtual reality] areas”. With support from Masdar Institute of Science and Technology in Abu Dhabi (in collaboration with MIT), InGlove has been given full use of the institute’s labs.
“We all think AR and VR are the future of communication.”
But there aren’t enough people who think like that here.
While InGlove might be being accelerated in the Middle East, they don’t see the region as their target market. They are heading for where they see a higher adoption rate of such new technology - the US.
“I certainly think AR is worth tracking closely,” says Omar Sati from Jordanian investor DASH Ventures. “I think the key element is how interactive the AR technology is. If people can interact with it, as opposed to it just being illustrative, like a hologram, for example, then the potential is limitless.”
Looking at how technological advancements without any obvious connection to medicine end up becoming invaluable to the sector, Abu Sitta points out that WhatsApp has become a major tool for doctors in Syria.
“We are witnessing the collapse of the majority of health sectors around the world,” he said to Wamda. “So we have to set up support mechanisms, and this is the next step in the telemedicine sector evolution.


